CHRONIC PANCREATITIS IN CHILDREN
Patient Education Material
Pancreas:
The pancreas a gland that lies across the back of your upper abdomen. Behind the stomach and guts (intestines) and in front of the spine. And just above the level of your belly button (umbilicus). Its shape is like a cylinder and about 15cm long and 3cm wide. The pancreas has two main functions.
- Exocrine function: It produces a fluid called “pancreatic juice” that flows through a small tube in the center of the pancreas called the pancreatic duct into your small intestine (duodenum). Pancreatic juice helps to digest the food so that the proteins, fats, and carbohydrates can be digested and then absorbed into the bloodstream and used for energy for other body functions.
- Endocrine function: Groups of special cells called ‘Islets of Langerhans’ are scattered throughout the pancreas. These cells make the hormones insulin and glucagon. The hormones are passed (secreted) directly into the bloodstream to control the blood sugar level in the body.
The bile duct carries bile from the liver and gallbladder. This joins the pancreatic duct just before it opens into the duodenum. Bile passes into the duodenum and helps to digest food.
Chronic Pancreatitis:
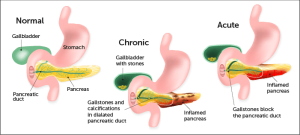
Chronic pancreatitis inflammation of the pancreas that worsens over time. It causes scarring and permanent damage to the pancreas.
The pancreas a large gland behind the stomach that makes enzymes (digestive juices) that travel to the upper portion of the digestive tract. where they help to digest food.
In a healthy pancreas, these enzymes do not become active until they reach the upper part of the digestive tract. But when the pancreas inflamed, the enzymes become active while they are still in the pancreas, and begin attacking the tissues inside the pancreas. These tissues become damaged and cannot produce new enzymes. Scar tissue develops over time and the pancreas shrinks in size. When that happens, the pancreas cannot produce enough enzymes needed for digestion.
Over time, this tissue damage can become permanent. The ability to digest food impaired and the pancreas cannot produce enough enzymes to help control blood sugar. At this point, the pancreatitis is considered chronic.
How common is Chronic Pancreatitis:
Chronic pancreatitis rare in children. It diagnosed at any age but is more common after the age of 10.
What causes Chronic Pancreatitis in children:
Causes of chronic pancreatitis in children may include:
- Gallstones or a blockage in the pancreatic duct.
- A metabolic abnormality, such as high levels of calcium in the blood.
- Heredity or genetics (passed on from family).
- Trauma to the pancreas.
Other causes include medication, an infection or another disease, such as cystic fibrosis. However, in many cases, the cause of chronic pancreatitis in children is unknown.
Problems associated with Chronic Pancreatitis:
The main problem for those with chronic pancreatitis is chronic pain. Chronic pancreatitis can cause serious complications, including:
- Dehydration or low blood pressure.
- Bleeding, tissue damage, and infection.
- Fluid-filled cavities (pseudocysts)in the pancreas. which can cause vomiting and fever.
- Injury to the heart, lungs, and kidneys or other organs. when digestive enzymes and toxins enter the bloodstream.
- Diabetes mellitus due to the loss of pancreatic tissue and cells that produce insulin.
- Fat not getting absorbed into the body which leads to fatty stools due to a lack of digestive enzymes.
- Diarrhea, bellyaches, bloating, and distension (a protruding belly).
Signs & symptoms:
Chronic pancreatitis begins with multiple episodes of acute pancreatitis. These episodes typically involve intense upper abdominal pain, vomiting, and nausea.
The most common symptom of chronic pancreatitis pain in the upper belly that much worse than a typical bellyache. A child may describe it as severe, or have trouble standing or sitting upright. The pain can be constant, come and go, and worsen after eating, especially after eating foods that are high in fat.
Another common symptom is weight loss. This due in part to not being able to absorb nutrition. In some cases, children avoid eating because it aggravates painful symptoms. Sometimes, pancreatitis can cause a loss of appetite, which leads to weight loss.
Other symptoms of chronic pancreatitis include:
- Nausea
- Vomiting (vomit may be yellowish, greenish or brownish).
- Diarrhea and oily bowel movements.
- Trouble digesting food and poor growth.
- Diabetes mellitus.
- Jaundice (yellow discoloration of the skin).
- In some cases, back pain or left shoulder pain.
How to diagnose Chronic Pancreatitis:
Because symptoms of chronic pancreatitis resemble those of other illnesses, diagnosing it can be challenging. Pancreatitis is sometimes misdiagnosed as constipation, heartburn, inflammatory bowel disease, or irritable bowel syndrome.
To diagnose chronic pancreatitis, a physician will perform a thorough physical examination. And ask questions about the child’s medical history. Tests may include:
- Blood tests to see how well the pancreas is functioning and check the pancreas enzyme levels. And to check the production of insulin and if the pancreas enzymes are high.
- Endoscopic retrograde cholangiopancreatography (ERCP), an imaging procedure used to examine the small intestine, pancreatic duct, and other parts of the gastrointestinal tract.
- A CT scan of the belly. This technology uses X-rays and computer technology to reveal signs of damage to the pancreas.
- An MRI (magnetic resonance imaging), which can show abnormalities in the pancreatic duct.
- Stool tests
- Genetic tests can identify a possible hereditary (inherited) cause.
Treatment of Chronic Pancreatitis:
There is no cure for chronic pancreatitis, but treatment can ease the symptoms and improve a child’s quality of life. It is important to treat chronic pancreatitis as soon as possible because repeated inflammation can cause permanent damage. Treatment options include:
- Taking pancreatic enzymes to aid in digesting nutrients.
- Following a special diet and/or taking vitamins to address the body’s inability to absorb certain nutrients.
- Surgically removing the gallbladder or pancreas.
- Taking medication to correct a metabolic imbalance.
- Undergoing endoscopic retrograde cholangiopancreatography (ERCP) to relieve a blockage that is causing pancreatitis.
Surgery:
Most children with chronic pancreatitis do not need surgery but an operation is sometimes needed. The common reason for surgery is for persistent bad pain that is not helped by painkillers or other methods. Improvement in pain occurs in about 7 in 10 patients who have surgery. The operation usually involves removing part of the pancreas. There are different techniques that remove different amounts of pancreas. The one chosen depends on the severity of the child’s condition, whether the pancreatic duct is blocked, and also on various other factors. Other operations may be advised in some cases – for example, removal of a large calcium stone that is blocking the main pancreatic duct.
Another procedure that may help in some people is to ‘stretch’ wide a narrowed pancreatic duct to allow better drainage of pancreatic enzymes. Surgery may also be needed if a complication develops. For example, if a blocked bile duct or pseudocyst develops. If the pain is persistent you may be offered a procedure to block the nerve supply to the area. Examples of treatments that involve this approach are coeliac plexus block and spinal cord stimulation. If you need surgery, then your surgeon will be able to discuss with you in detail the type of operation you need.
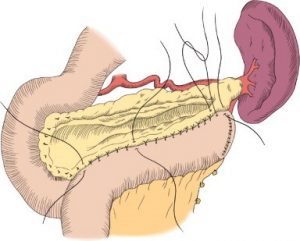
Total Pancreatectomy and Islet Cell Autotransplantation:
In rare cases, a child may undergo a surgery called a total pancreatectomy and islet autotransplantation (TPIAT). This involves removing the entire pancreas and reconstructing the gastrointestinal tract. After the pancreas is removed, it is taken to an islet laboratory where the islet cells are extracted. These cells are responsible for producing insulin and other hormones. The islets are then transplanted into the patient’s body, where they continue to perform essential functions of the pancreas.
Although TPIAT is a complex surgery, the operation can be life-changing for patients in whom previous interventions have not resulted in relief from the painful symptoms of pancreatitis.
Pain Control:
Chronic pancreatitis can cause intense upper belly pain. Minimizing this pain and helping your child cope with it is a high priority. A pediatric pain specialist can offer medication and strategies to help your child cope with painful symptoms while also minimizing the use of narcotics. A pain psychologist can also help by providing coping strategies to deal with the pain.
The outlook of children with Chronic Pancreatitis:
Not all children who experience acute episodes of pancreatitis will develop chronic pancreatitis, but some will.
Unfortunately, chronic pancreatitis is a lifelong condition, although symptoms sometimes come and go. Patients should see their doctor on a regular basis to evaluate their condition, ensure that they are getting enough nutrition, and discuss treatment options. The doctor will provide endocrine testing on a regular basis to identify any issues related to glucose tolerance or the development of diabetes.
More about surgery:
Children with chronic pancreatitis may be at an increased risk of developing pancreatic cancer. The degree of risk depends on the underlying cause of pancreatitis, family history, and the type of genetic involvement.

